What is regulatory supervision? (education context)
Regulatory supervision is a
professional decision-making process nurses use when students perform client care activities that require nursing knowledge, skill, ability, and judgment. It protects clients while supporting student learning.
Applies to: student nurses in clinical placements and, in some settings, students from other regulated health professions when nurses supervise their entry-level practice.
Bottom line: clinical practice consolidates learning. Students are required to have gained sufficient knowledge, skills, ability, and judgment to perform the activity under supervision through their program.
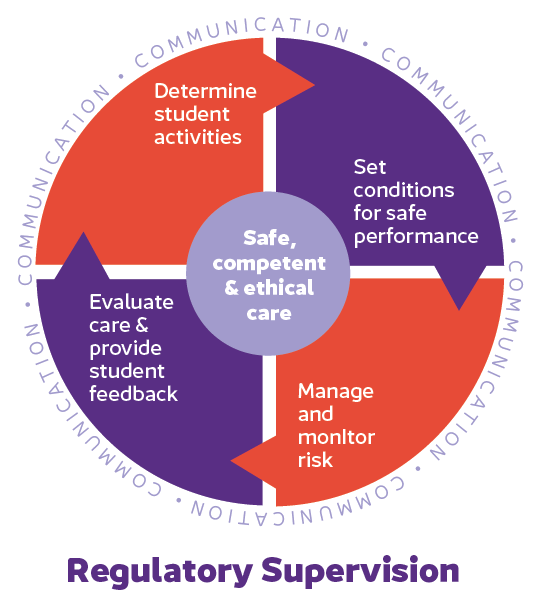
Regulatory supervision process
“I've done this in lab…"
Use this scenario to follow along as you learn each step of the supervision process.
Maya, a third-year nursing student, confidently offers to perform a complex wound dressing change 'independently'. The wound is deep, slow to heal, and requires sterile technique.
You have not yet confirmed Maya's knowledge, skill, ability, and judgment.
What should you do next?
Step 1 – Determine student activities
In the moment: A student offers to do an activity.
Your goal: decide what the student can do safely right now based on student knowledge, skill, ability, and judgment, and risk.
What you do
- A. Confirm the activity fits you (the supervising nurse)
Proceed only if:
- The activity is within your scope of practice, and
- The activity is within your individual competence
When supervising across professions, ensure the activity fits your scope/competence and aligns with the student's program competency expectations.
- B. Confirm the student's readiness for the specific activity
Confirm what the student has gained sufficient knowledge, skills, ability, and judgment through their education program (or equivalent) to safely perform the activity. Use reliable sources such as:
- Program expectations and skill verification/sign-offs
- Instructor or preceptor feedback (education context)
- Observed performance in clinical practice
- The student's understanding of indications, steps, safety checks, and limits
- Documentation of prior supervised practice (where applicable)
What you can say (quick script)
- “Tell me what you've done with this in practice and what you'd do if the client's condition changes."
- “Walk me through the safety checks and where you'd pause for me."
Common decision traps
-
“They've done it in lab." Lab practice ≠ readiness for complex/high-risk client situations.
-
Staffing pressure. It doesn't change what's safe.
- C. Confirm client consent (when possible)
Before the student participates, obtain the client's consent when possible and document according to employer policies.
Maya has practised wound care in lab but has done only one complex dressing change in practice. Because the wound is complex, you decide she will not complete the dressing change independently.
Step 2 – Set Conditions for safe performance
In the moment: You've decided the student can participate—but not independently.
Your goal: make performance safe by setting conditions and a supervision plan.
In Step 2, you complete two linked actions:
Set the conditions by defining what the student can do, what requires nurse involvement, and what safeguards must be in place.
Develop the supervision plan by confirming the supervision level and where and when supervision will occur, communication and escalation expectations, and how supervision will be maintained across the shift.
- Supervision options (choose based on risk/student readiness)
- What you base it on
- What you can say (quick script)
Because the client's wound is complex, you choose direct supervision and set clear conditions.
- Set the conditions
Maya may:
Maya does
not complete the full dressing change independently. You are present for sterile/high-risk steps and to manage unexpected findings.
- Supervision plan
Step 3 – Manage and monitor risk throughout care
In the moment: the student is performing and the situation may evolve.
Your goal: protect the client by anticipating risk, stepping in early, and updating conditions as needed.
- What you do
- What you can say (quick script)
When Maya breaks sterile technique, you intervene immediately and guide corrective steps.
Step 4 – Evaluate care and provide feedback
Review the care provided by the student, assessing whether all planned steps were completed safely and effectively and client response and outcomes.
Provide constructive, timely feedback, focusing on clinical reasoning and communication. Guide the student in identifying what they would do differently next time, supporting their learning and accountability.
- Quick debrief with Maya (1–2 minutes)
Closing: Support safe student participation by setting clear conditions, stepping in early when risk appears, and updating the plan for next time.
If something goes wrong
If a student's action harms (or could harm) a client, the nurse:
- Takes immediate steps to ensure client safety
- Notifies appropriate supports (e.g., charge nurse, instructor, employer/manager as applicable)
Supports the student to follow incident reporting processes (practice setting, educational institution, and/or employer processes, as applicable)
Key point: You may not be accountable for events you could not reasonably foresee, but you are accountable for appropriate supervision decisions, conditions, communication, and professional judgment.
Communication that supports safe learning
Nurses who provide regulatory supervision:
- Clarify roles and responsibilities with the student, instructor/faculty, and other health professionals as needed
- Support the student to speak up about risks and ensure reporting occurs per policy
- Ensure the student is aware of relevant BCCNM standards and practice setting policies and procedures
- Ensure the student uses the appropriate title when communicating and documenting
- Address professional practice issues promptly and constructively (e.g., boundaries, discrimination)
- Communicate respectfully and act to create a safe learning environment
- Reflect and take action to support culturally safe learning and client care in alignment with the
Indigenous Cultural Safety, Cultural Humility and Anti-Racism practice standard
- The 4Q check: Know before you permit
Use before approving any activity:
1. What knowledge, skills, ability, and judgment has the student gained through their education program?
2. Is this activity within my scope and individual competence?
3. What are the risks for this client in this situation?
4. What conditions and level of supervision are required, and how will I evaluate outcomes?
Apply your understanding: Liam's scenario
Consider the following scenario and apply your understanding:
A client is 8 hours post abdominal surgery and reports increasing pain, new nausea, and difficulty taking deep breaths. Earlier vitals were stable.
Liam says, “I can do the full postoperative assessment and give the analgesic. I've learned this in school and have done this several times."
You don't yet know Liam level of knowledge, skill, ability, or judgment with early post-op clients or changing conditions.
Step 1 – Determine student activities
Before Liam performs any client care activity, what information do you need to make a safe supervision decision?
- A. Whether Liam feels confident completing the assessment independently.
-
Incorrect. Being confident doesn't necessarily mean Liam possesses the necessary knowledge, skills, ability, or judgment.
- B. How many times Liam completed the assessment in lab and how confident he is now.
-
Incorrect. Lab experience alone is insufficient for higher-risk clinical situations.
- C. What Liam has demonstrated in clinical practice: documented skills, experience with early postoperative clients, experience with changes in condition, and current learning needs.
-
Correct. Safe supervision requires reliable evidence of what Liam can safely do in practice.
- D. Whether the unit is short-staffed and could benefit from Liam working more independently.
Incorrect. Staffing pressures do not determine what is safe when supervising students.
Step 2 – Set conditions
Based on Liam's request and the client's condition,
what conditions and supervision plan are most appropriate?
- A. Liam completes the full postoperative assessment and administers the analgesic independently because he has done similar activities before.
Incorrect. Prior exposure alone does not justify independent performance, especially with changing condition.
- B. Liam completes the full assessment alone and reports back immediately with findings.
Incorrect. Reporting back after the fact is not enough when the client may be changing.
- C. Liam completes selected components of the assessment with you present, you interpret findings, determine next steps, and decide whether/what medication is appropriate.
Correct. The client has new postoperative symptoms, so you set limits on what Liam does and remain directly involved in clinical judgment and decisions.
- D. Liam does not interact with the client until he completes more formal training.
Incorrect. The safest approach is participation with conditions—not unnecessary exclusion.
Step 3 – Manage and monitor risk
During the assessment, Liam notes the client's heart rate has increased and abdominal guarding is present. What should the supervising nurse do next?
- A. Tell Liam to continue and update you when he finishes.
-
Incorrect. Concerning changes require immediate nurse involvement.
- B. Ask Liam to recheck vital signs later to see if they improve.
-
Incorrect. “Wait and see" is unsafe with new concerning symptoms.
- C. Encourage Liam to troubleshoot independently to build confidence.
-
Incorrect. Higher-risk situations are not appropriate for independent student decision-making.
- D. Step in immediately to reassess the client, determine next steps, escalate appropriately, and guide Liam through safe care.
-
Correct. These signs may indicate postoperative complications; you intervene promptly.
Step 4 – Evaluate care and provide feedback
Review the care Liam provided, assessing whether all planned steps were completed safely and effectively and client response and outcomes.
- Quick debrief (2–3 minutes)
When appropriate, debrief with Liam:
Closing: This case shows how to support safe student participation when a client may be deteriorating: confirm readiness, set clear conditions with the appropriate supervision level, step in early when new findings emerge, and update the plan for next time.